Keratoconus
What is Keratoconus?
Keratoconus is a type of corneal ectasia characterized by thinning and bulging to the cornea, the clear dome-like structure on the front of the eye. The condition typically occurs in patients ages 10-25 and continues to progress slowly over 20 year or more. Although the cause of keratoconus is unknown, it is thought to have both genetic and environmental factors. Keratoconus is more common among patients with other systemic conditions such as atopy, sleep apnea, and other connective tissue disorders.
Many patients with Keratoconus slowly develop symptoms of blurred or distorted vision and light sensitivity that is typically worse in one eye than the other. They may also note a need for frequent changes to their glasses or contact lens prescriptions. In severe stages of the disease, sudden worsening to vision or clouding to vision can occur.
Corneal Cross-Linking
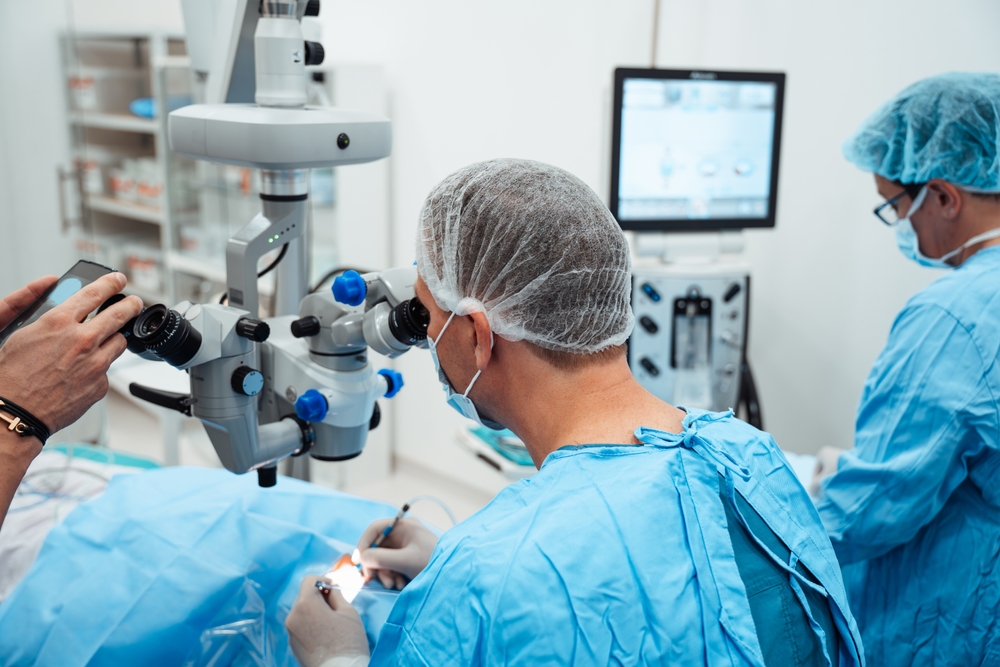
Corneal cross linking, or CXL, is a procedure used to stabilize the cornea in patients with ectasia. CXL utilizes riboflavin and ultraviolet light to strengthen the structural layer of the corneal called the stroma. It is this strengthening of the stromal layer that inhibits further progression of ectasia. The procedure involves first removing the epithelium, or front layer from the cornea. The eye is then soaked with riboflavin solution before initiating ultraviolet light. Lastly, a bandage soft contact lens is placed in the eye and eye drops are used for several days postoperatively. The procedure is done with topical anesthesia and usually lasts around one and a half hours.
Corneal Transplant
Corneal transplant for Keratoconic patients is needed when a patient’s vision is no longer correctable with glasses or contact lenses due to severe scaring or steepening of the cornea. Corneal transplant is also considered when the cornea becomes extremely thin and has the possibility to perforate. The procedure involves cutting out the irregular portion of a patient’s cornea and replacing it with donor tissue. Full-thickness vs partial thickness transplants are used for keratoconus. Your doctor will determine the best type of graft to use based off your in-office evaluation. Vision after corneal transplant surgery typically takes months before stabilizing to the point that patients are able to update glasses and specialty contact lens prescriptions. Eye drops are used for many months postoperatively with the possibility that patients may need to be on eye drops indefinitely to prevent rejecting the transplant.